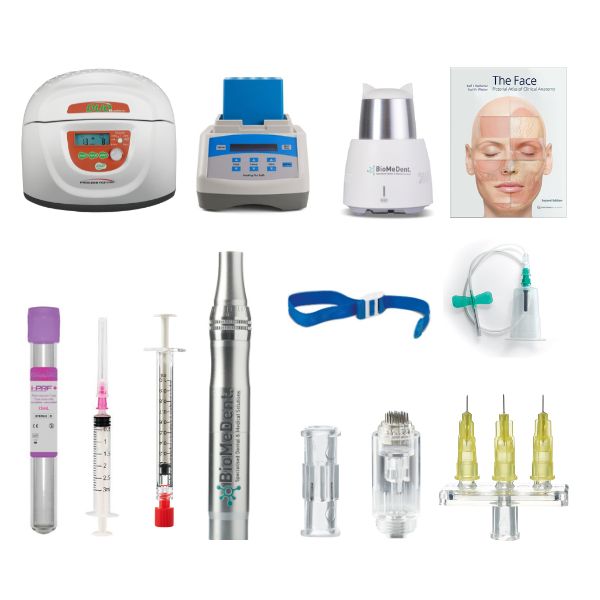
Biomedent is the official distributor of Process for PRF® in Australia & New Zealand
Regulatory Status:
ARTG-listed Class IIa. Official Process for PRF® product, developed by Dr. Choukroun creator of the Process for PRF® (Platelet Rich Fibrin) technique (A-PRF, i-PRF, & S-PRF).
The concept of PRF (Platelet-Rich Fibrin) is based on the centrifugation of whole blood without anticoagulants (J. Choukroun et al., 2001). During centrifugation, a fibrin clot is formed that contains a concentration of platelets and white blood cells.
Platelet-Rich Fibrin (PRF) is an autologous platelet concentrate used in medical and dental procedures for tissue regeneration and healing support.
Composition:
PRF is derived from the patient’s own blood, which is centrifuged to separate the plasma and form a fibrin clot. PRF does not require anticoagulants or bovine thrombin.
Formation:
Centrifugation allows the formation of a fibrin clot containing platelets, white blood cells, and other blood components. These components are part of the natural blood composition and can be handled and applied in clinical procedures.
Intended Use:
PRF is intended for use by qualified healthcare professionals in clinical procedures that involve tissue repair and regeneration support. Its applications are limited to professional use and should be applied according to clinical protocols.
PRF vs PRP: Key Differences:
Platelet-Rich Fibrin (PRF) and Platelet-Rich Plasma (PRP) are both autologous platelet concentrates, but they differ in composition and preparation:
Anticoagulants: PRF is prepared without anticoagulants, allowing natural fibrin clot formation, whereas PRP typically requires anticoagulants.
Fibrin Matrix: PRF forms a three-dimensional fibrin network, which acts as a scaffold for platelets and white blood cells, supporting gradual release of growth factors. PRP usually remains in a liquid form.
Cellular Content: PRF contains higher concentrations of white blood cells and platelets within the fibrin matrix, which may contribute to tissue handling and cellular signaling in surgical protocols.
Handling: PRF’s clot or membrane form may be easier to handle in certain surgical or grafting applications compared to liquid PRP.
Applications in Dentistry:
Periodontal Surgery: PRF can be used to manage soft tissue and periodontal procedures.
Oral Surgery: PRF can be applied during dental extractions and other oral surgical procedures.
Implantology: PRF may be used in implant-related procedures, including bone grafting and sinus augmentation.
Bone Grafting and Ridge Augmentation: PRF may be used in combination with graft materials to support bone handling.
Endodontics: PRF may be used during procedures addressing periapical tissue.
Applications in Medicine:
Orthopedics: PRF may be used to handle and support tissues in orthopedic procedures.
Plastic and Reconstructive Surgery: PRF may be applied in surgical procedures to manage tissue layers.
Dermatology: PRF may be used in procedures addressing scalp or skin tissue.
Cardiovascular and Ophthalmology: PRF may be handled during procedures involving vascular or corneal tissues.
Advantages for Professional Use:
Autologous: Derived from the patient’s own blood.
Simple preparation: PRF can be prepared using standard centrifugation equipment.
No chemical additives or anticoagulants required.
Important Notice: PRF is intended for use by licensed medical and dental professionals only. Clinical use must comply with institutional protocols and TGA regulations. The product is listed on the ARTG and classified as Class IIa medical device.
Useful Links & Research
Media Library:
Free Online Lecture on PRF by Dr Joseph Choukroun MD - Creator of the Process for PRF Technique:
Paid PRF Courses:
Research:
National Library of Medicine - National Center for Biotechnology Information
- Role of Platelet rich fibrin in wound healing: A critical review
- Platelet-Rich fibrin: A second generation platelet concentrate and a new friend of oral and maxillofacial surgeons
- Platelet-rich Fibrin PRF versus Platelet-rich Plasma PRP: A Study to Assess Efficacy as a Regenerative Medicine Strategy for Chronic Cutaneous Ulcers
- Fluid Platelet-Rich Fibrin (PRF) Versus Platelet-Rich Plasma (PRP) in the Treatment of Atrophic Acne Scars: A Comparative Study
- Evaluation of the Effect of Platelet-Rich Fibrin Matrix in the Correction of Periorbital Wrinkles: An Experimental Clinical Trial
- Injectable platelet-rich fibrin for facial rejuvenation: A prospective, single-center study
Oral & Maxillofacial Surgery Journal
Research Gate Publication
International Journal of Dermatology and Venereology